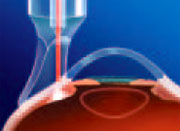
 Medications, lasers, and incisional surgery are used to lower the intraocular pressure to treat patients with glaucoma in order to prevent progressive optic nerve damage. One technique that is required at times is ‘ablation’ of the ciliary body – the portion within the eye that produces the aqueous humour. This procedure partially damages the ciliary body so that it makes less of the fluid that is responsible for the pressure in the eye. It tends to be saved for times when other surgical interventions have all failed. It used to be only for eyes that were almost completely blind but by titrating the dosage, it can be an option even if there is some vision intact. There is a related procedure called endoscopic cycloablation which is a more precisely delivered treatment but requires a visit to an operating room as it is performed by inserting a delivery probe into the eye.
Medications, lasers, and incisional surgery are used to lower the intraocular pressure to treat patients with glaucoma in order to prevent progressive optic nerve damage. One technique that is required at times is ‘ablation’ of the ciliary body – the portion within the eye that produces the aqueous humour. This procedure partially damages the ciliary body so that it makes less of the fluid that is responsible for the pressure in the eye. It tends to be saved for times when other surgical interventions have all failed. It used to be only for eyes that were almost completely blind but by titrating the dosage, it can be an option even if there is some vision intact. There is a related procedure called endoscopic cycloablation which is a more precisely delivered treatment but requires a visit to an operating room as it is performed by inserting a delivery probe into the eye.
Until the early 1990’s, the device used to provide this treatment was a freezing (cryo) probe. This is still used on some occasions but has been replaced mostly by the use of a laser to concentrate the energy so that it is only being delivered to its target rather than to the surrounding tissues. The potential side effects using the older cryotherapy included:
- the need for further surgery;
- loss of vision;
- pain;
- eventual shrinkage of the eye (phthisis);
- corneal or ocular surface irritation;
- intraocular inflammation, and;
- the usual risks of anaesthetic (as injection required around the eye.)
The newer cyclophotocoagulation delivers the same effect as the cryotherapy but with fewer side effects. In fact, the biggest risk with this procedure is that of insufficient treatment resulting in the need to repeat it. There is still the risks of the anaesthesia as well as of the inflammation post-operatively.
(c) 2010-2011 Robert M Schertzer, MD, MEd, FRCSC with information from OMIC
