 What is SLT?
What is SLT?
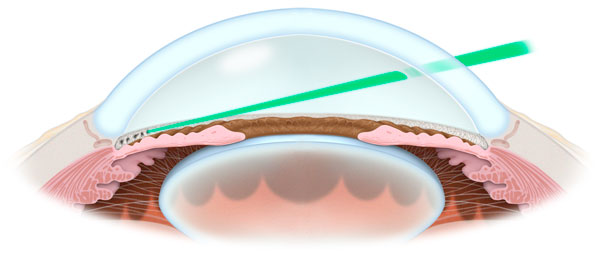
Selective laser trabeculoplasty (SLT) is a laser surgical procedure used to help lower intraocular pressure (IOP) of patients with open-angle glaucoma. SLT is used to treat the eye’s drainage system, known as the trabecular meshwork—the mesh-like drainage canals that surround the iris. Treating this area of the eye’s natural drainage system improves the flow of fluid out of the eye, helping to lower the pressure.
The laser used in SLT works at very low levels. It selectively treats specific cells, leaving untreated portions of the trabecular meshwork intact. For this reason, SLT, unlike other types of laser surgery, may be safely repeated many times. The ultra-brief shock waves delivered to the drainage channels result in the release of an additional amount of a substance typically found in the eye, matrix metalloproteinases, which help clean the meshwork so that it functions better.
How the laser is performed
SLT is performed at the West Coast Glaucoma Centre by Dr Schertzer. The laser machine resembles the examination microscope that your ophthalmologist uses to examine your eyes during each office visit. The procedure itself usually takes just a few minutes per eye. The Ophthalmic technician will place a drop of an anti-glaucoma medication in your eye to prevent a pressure spike after the procedure. An anesthetic drop is instilled in your eye before touching a mirrored lens to your eye that is coated with a lubricating tear gel. You will experience a flash of light with each laser application. Most people are comfortable and do not experience any significant pain during the procedure, although some may feel a slight pressure in the eye.
 Some people will need to have their pressure checked within one hour following the laser treatment, as there is a risk of increased IOP after the procedure. An eyedrop instilled prior to the treatment almost always prevents this pressure spike.
Some people will need to have their pressure checked within one hour following the laser treatment, as there is a risk of increased IOP after the procedure. An eyedrop instilled prior to the treatment almost always prevents this pressure spike.
Argon Laser Trabeculoplasty (ALT) – the older way
With the older modality, which is still quite effective and in use (Argon Laser Trabeculoplasty), on rare occasions, the pressure in the eye increases to a high level and does not return to normal. If this happens, patients may require surgery in the operating room to lower the pressure. This has not been my experience with the SLT technique at all.
Most people notice some blurring of their vision after the laser treatment. This typically clears within ten minutes and is due mainly to the tear gel used on the lens that comes into contact with your eye during the procedure. The chance of your vision becoming permanently affected by this laser procedure is extremely small.
Most patients can resume normal daily activities the day after the laser procedure. You may need to use anti-inflammatory eyedrops after the procedure for a few days if you are sensitive to light or your eyes become red. However, the use of anti-inflammatory drops risks reducing the effectiveness of the treatment.
Risks associated with SLT
- increased pressure in the eye, possibly requiring medication, in a small proportion of patients in the first hour after the treatment;
- inflammation in the eye;
- scratching the cornea from the lens or tonometer used to measure the eye pressure;
- failure to adequately lower the eye pressure; and
- need for repeat laser treatment.
Recovery
It will take up to 6 weeks to determine how much SLT will lower your eye pressure. You may require additional laser or glaucoma drainage surgery to lower the pressure if it is not sufficiently lower after the first laser treatment. Patients are seen at the 1-week mark to ensure there is no inflammation and then at the 6-week mark to assess the effectiveness of the treatment.
Most patients must continue to take medication to control and maintain their IOP; however, surgery can lessen the amount of medication needed.
While some people may experience side effects from medications or surgery, the risks associated with these side effects should be balanced against the greater risk of leaving glaucoma untreated and losing your vision.
© 2025, 2021,2020, 2015, 2009 Robert M. Schertzer, MD, MEd, FRCSC based on 2007 The American Academy of Ophthalmology
